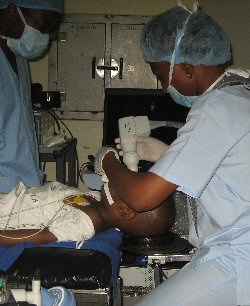
If found early, childhood eye cancer is curable with highly specialised medical care.
Lack of nationally co-ordinated retinoblastoma care places great burdens on families and health systems, prevents efficient use of available resources, and causes children to die or lose eyes needlessly. We have introduced nationally agreed guidelines, pathology, treatment, patient records, imaging and artificial eyes that give each child vital personalized care.
The Challenge
Treatment of retinoblastoma frequently fails to achieve best possible outcome for the child and family due to lack of clearly defined management plans.
This happens in most countries worldwide, regardless of economic development or available resources, but it is a particular challenge in developing countries.
Management of retinoblastoma includes referral, screening and diagnosis, staging, treatment, genetic testing, follow up care and psychosocial supports.
Our Solution
Using the Canadian Retinoblastoma Guidelines as a model, the KNRbS group has developed Best Practice Guidelines appropriate for the resource-limited setting. Agreed, evidence-based recommendations enable common standards of care for children and families across Kenya; from referral and diagnosis through treatment and follow-up.
The guidelines were developed collaboratively over five years. Annual meetings of the Kenyan National Rb Strategy Group facilitated consensus agreement and comprehensive national ownership. Our international team provided knowledge and expertise in guideline writing to facilitate appropriate editing and formulation of the Kenyan document.
The Kenyan National Retinoblastoma Care Guidelines were adopted by the government in September 2014 and their recommendations are now being implemented across the country.
Over the coming years, our team in Kenya and internationally will follow a comprehensive review process to ensure each of the guideline recommendations is being implemented effectively and positively impacting children, their families, survivors and those who care for them.
Impact of Guidelines
Kenya’s nationally co-ordinated approach to retinoblastoma is improving access to vital medical care. Medical professionals are better equipped to provide optimal care for children and their families. This is relieving pressure on limited medical resources. Many of the financial, physical and social burdens that have crippled families are already significantly reducing, and some may be eliminated completely in the coming years. Ultimately, many more children will overcome their cancer.
Retinoblastoma in Africa can be cured. Our solutions strengthen local capacity to provide effective care, reducing the strain on financial, human and material resources.
Children have a greater chance of cure and parents have hope. Medical professionals also feel more positive and confident about treating patients with this difficult cancer and communicating with their families.