If You Tell Them, They Will Know
Raising awareness of retinoblastoma signs can save lives, eyes and sight.
Monday May 11, 2020
Strabismus (turned eye) and leukocoria (white pupil) are the most common early signs of retinoblastoma. Sandra Staffieri, Rb Care Co-ordinator at the Royal Children’s Hospital, Melbourne, explores why parent and healthcare provider awareness of these signs is vital to early diagnosis of childhood eye cancer.
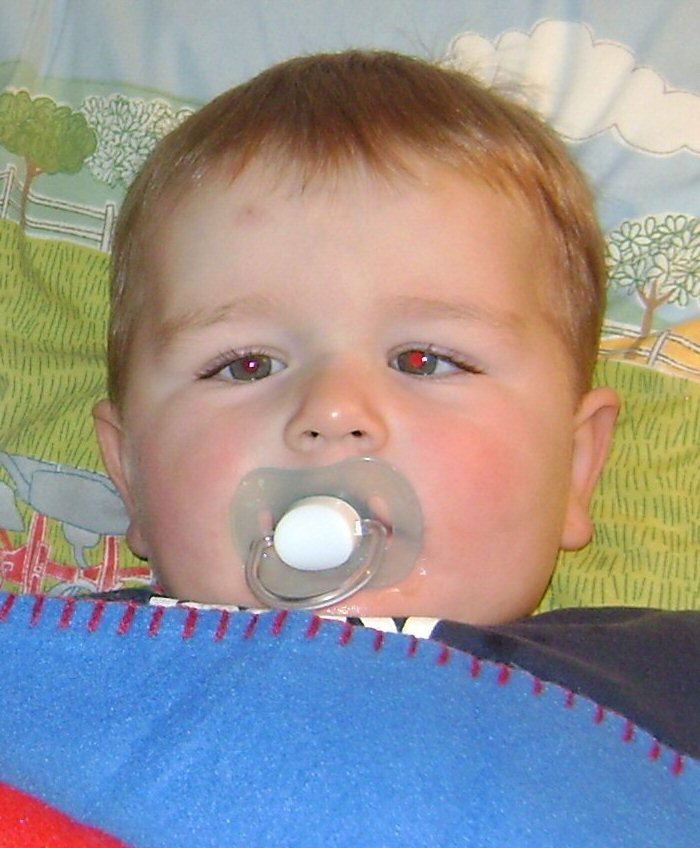
Examples of leukocoria (white pupil) and strabismus (turned eye)
The experiences of parents whose children have been diagnosed with retinoblastoma tell us that more awareness and education is needed about the early signs of this cancer.
“After our daughter was diagnosed with bilateral Rb at 18 months, we traced the white reflex back in photos to 11 months old. We had no idea about Rb or its symptoms before the diagnosis. This is such a simple sign for parents and photographers to look for, and easy to explain to people…We would have remembered to look for this sign if we had been educated about it. Maybe our daughter would still have both eyes if she had been diagnosed when the white glow was first obvious in our family snaps.”
But it is not only parents who need educating… healthcare providers need reminding too…
“What is it with doctors who don’t listen to parents’ concerns? We saw the white eye glow so early, in photos and with our own eyes in dim light. We went to our family doctor repeatedly. We spoke to the pediatrician and to the breastfeeding nurse. None of them looked in her eye and all of them said she was fine, even when I showed the doctor the photos. …I had already searched online, I knew in my gut that she had Rb but they just told me I was a neurotic first-time mom.”
Why Raise Awareness of Retinoblastoma?
Fact: timely diagnosis of retinoblastoma is critical – a child’s life can depend on it!
Retinoblastoma is the most common eye cancer of infancy and early childhood. Tumours usually begin to develop in most affected children before their second birthday. We know that diagnosis and treatment before this cancer extends beyond the eye is critical to saving a child’s life, let alone their eyes or vision. By its very nature, retinoblastoma remains cocooned within the eye for quite some time, providing a unique opportunity to diagnose and treat it early, with the potential for the best possible outcome – Survival and Sight.
The most common presenting signs of retinoblastoma are white pupils (leukocoria) or a crossed/turned eye (strabismus/squint). These early signs are “silent” in that there may be no other clue that the child has an eye problem, other than what their parents/caregivers observe. When a child has leukocoria or strabismus but continues to behave normally and feel “well”, it can be easy to dismiss.
Whereas acute problems such as poor vision or eye pain, or more obvious symptoms such as a red eye, change in eye colour or pupil size, or even a protruding eye, may be more likely to prompt parents to see a doctor or health nurse. But these more obvious symptoms occur when the disease is advanced, and possibly already outside of the eye.
During the COVID-19 pandemic, lockdown and physical distancing has posed limitations on seeking medical help. Despite this unprecedented era, if as a parent you are concerned about your child’s eyes, DO NOT WAIT to seek advice. Take photos, and call your doctor, health nurse or optometrist for advice.
Fact: parents or caregivers are the most likely to notice there might be a problem with their child’s eyes – simply by what they observe!
“…children with visual problems generally do not complain, they are dependent on their parents identifying and acknowledging that there is a problem…”
Delayed diagnosis of retinoblastoma, and the consequences, is a well-documented problem worldwide. It is known to occur primarily because parents do not recognise or respond to the early signs. Furthermore, when the parent does seek advice, the healthcare provider may not listen to parent concerns or adequately examine the child.
So, raising awareness of these early signs for both parents and healthcare providers would seem to be the most obvious way to reduce delays in diagnosis.
Fact: raising awareness of signs or symptoms of almost any disease reduces delays in diagnosis and treatment, and improves outcomes – retinoblastoma is no different!
Honduras Leads the Way
Honduras is a low-middle income country in Central America. Historically, a high rate of children presented with advanced retinoblastoma, particularly with cancer extending beyond the eye (extraocular disease). As a direct result, survival of children with eye cancer was poor. Recognising that survival could be improved by raising awareness of retinoblastoma early signs and re-educating health providers in the community, an awareness campaign was launched.
So, between the years 2003-2005, a widespread awareness campaign was developed. Posters were displayed in community health centres highlighting that white pupils in children was a problem not to be ignored. The message was repeated through television and radio commercials. The information provided included a “call to action” for parents, encouraging them to speak to their doctor or nurse if they observed a white pupil in their child.
A poster used during the Honduras awareness campaign.
A nurse educates parents about retinoblastoma during their routine visit to a vaccination centre in Honduras.
At the same time, local health-care workers were re-educated about white pupils. Training ensured that if a parent reported observing this phenomenon in their child, they would be referred promptly to the appropriate medical specialists for assessment. The campaigns were inexpensive and attracted philanthropic support.
As a direct result of these efforts, within 18 months of the campaign, the survival rate of children with retinoblastoma in Honduras skyrocketed from 14% to 48%. This was simply because parents were presenting when they noticed the white pupil, and not when signs of extraocular disease were observed, and importantly, healthcare providers listened to them.
Published in the medical literature in 2007, this landmark study clearly demonstrated that “If you tell them, they will know”. The campaign strategy was simple – provide information that could be understood, motivate parents to be vigilant, and give them instructions on what to do. The posters were displayed in community centres where parents would come to have their child vaccinated – ensuring the right message at the right time to the right people. Also critical was the education of the healthcare providers to make sure that parents reporting white pupils were listened to and their concerns taken seriously.
This study is regularly promoted as an example of how simply raising awareness among parents and healthcare providers about the significance of white pupils can make a huge impact on the lives of children and their families – it doesn’t matter that the disease is rare.
This strategy has been adopted in other countries around the world, and social media is increasingly used to promote the health message – and we need to continue this approach.
How Can We Detect Retinoblastoma At The Earliest Possible Time?
Children with a Family History of Retinoblastoma…
Some children will have a family history of retinoblastoma. This history may alert the healthcare provider to ensure the baby is examined regularly from birth so that any small tumours can be diagnosed and treated early using treatments that safely save eyes and perhaps vision. If we look at the research, children with familial retinoblastoma who have early screening are more likely to not only survive, but retain their eyes. Their vision however will depend on exactly where in their eye the tumours are, and what treatments are needed to control the disease.
With specialised imaging, either whilst the baby is still in the mother’s womb or after the baby is born, retinoblastoma doctors can diagnose tumours very early. Even if these specialised imaging techniques are not available everywhere around the world, regular examination of the child’s eyes alone can detect very small tumours, giving that child the best chance of saving their eyes, and good vision.
What should I do if I had Rb or know that I carry the RB1 mutation?
- If you are planning a family, ask your doctor or health nurse to refer you to discuss genetic counselling and early screening for your baby.
- If genetic testing is available where you live, arrange this early as testing can take time. This will enable the results to be helpful from the very beginning.
- If your baby will need early screening after birth, ensure there will be enough time to plan this with the medical team that has experience caring for children with retinoblastoma.
But what about children who do not have a family history of retinoblastoma? How can they be diagnosed early?
Harry’s cancer was detected during a routine eye exam under anaesthetic, and he needed only laser treatment because of his early diagnosis. In contrast, his older sister, Katy, was diagnosed at one year old, when her parents noticed a white glow in her eye in certain light. She endured years of intensive therapy in the battle to protect her life and save some sight. Read their story.
Children without a Family History of Retinoblastoma…
Families need to rely on one of two ways of having their child’s cancer detected:
- Eye-screening examinations at birth and during childhood
- Parental recognition of developing signs or symptoms that will prompt them to see a healthcare provider, and the provider’s awareness to take them seriously.
White reflex is often not visible with a routine red reflex eye exam, and similarly does not appear in every photograph. This depends on the size, number and location of tumours within the eye, and the angle at which light enters the eye. The child in these three photos was diagnosed with cancer in both eyes.
What Eye-Screening Tests Can Be Done?
Examination of the Red Reflex
You will be familiar with the ‘red eyes’ that we see in photographs. This occurs, when light is shone into the eye, and is reflected back from the healthy retina as a characteristic red-orange glow.
This phenomenon is actually used as a test to screen babies when they are born. The doctor or health nurse will shine a light from a special instrument (ophthalmoscope) into the baby’s eyes and examine their ‘red reflex’. If anything blocks the passage of light into the eye (such as a cataract) or any lump inside the eye (such as retinoblastoma or Coats disease) the red reflex will appear different to the characteristic red-orange glow. The appearance of the red reflex however can vary with ethnicity – lighter and brighter in Caucasians and darker in children of Asian and African descent. This variation can cause confusion and uncertainty to the untrained eye.
Examples of red reflex in light and dark eyes.
The Red-Reflex Test in Routine Eye-Screening
In many countries, the Red-Reflex Test is used routinely to examine all babies at birth for significant eye problems. Research studies have shown that the red-reflex test is very good at detecting cataracts in babies but is less useful when screening for retinoblastoma at birth for a few reasons.
- In a newborn, the tumours would usually be too small to give an abnormal result.
- Absence of retinoblastoma at birth does not mean it will never develop.
- Not all retinoblastoma will be in the same position within the eye. So, only examining a small, central portion of the retina, as is done with the red-reflex test, could miss small tumours that are present in more peripheral parts of the retina.
Despite these misgivings, all the guidelines that mandate red-reflex testing in newborns report this test as being critical for detecting retinoblastoma. In many countries, the red-reflex test is only ever done once – at birth. This can give a false sense of security to the parents or even the healthcare provider that there is no retinoblastoma, and that there never will be. But retinoblastoma can develop at any time up until the child is about 5 years of age. So, doing this test at birth will not detect retinoblastoma that usually develops some months, or even years, later.
The Red-Reflex Test as a Clinical Examination
Apart from being used in eye screening at birth or during childhood, . When a parent visits a health care provider because they have seen a white pupil, or they have noticed a crossed or turned eye in their child, the red-reflex test is a quick and non-invasive examination that helps the doctor to decide whether the child needs to be examined by an eye specialist urgently.
Ideally, the test should be done in a darkened room so the pupils become larger and more of the retina can be seen.
Other ‘Screening’ Opportunities
In most countries vision screening is conducted at the very least before a child starts school, which can be anywhere from 4-6 years of age. Some children with retinoblastoma have been initially detected this way, but most children will develop the cancer well before this age. Large scale vision screening can be very helpful for diagnosing vision problems, but we cannot rely on this screening to diagnose retinoblastoma at the earliest possible opportunity.
Further complicating matters is the differing opinion globally about what type of eye or vision screening should be done, by whom and how often. This is often dictated by the cost of repeated screening, the resources available, how likely a problem will be detected, and whether earlier detection will make a difference to the patient or to health care resources.
For retinoblastoma, which is rare, large scale screening in the currently available programs is just not efficient. In the future we hope better, more efficient and cost-effective ways will become available to screen widely and frequently for a rare disease.
For Now, We Have To Rely On Raising Awareness…
So, we have come full circle to acknowledging we cannot rely on ‘screening’ alone to detect retinoblastoma early, to recognising the importance of educating parents and healthcare providers on the significance of white pupils and crossed eyes in children. To ensure these signs are not dismissed – even if they are seen only some of the time or in different lighting conditions, or only in a photo but not when looking directly at the child’s eye, we need education and awareness.
I am Concerned – What Should I Do?
What should I do if I think I see a white pupil or a crossed-eye in my child?
- If you can see a white pupil with your naked eye, see your doctor promptly!
- If you see a white pupil in ANY photos, retake your photos using the PhotoRED technique and / or CRADLE app, and see your doctor promptly if you are still concerned.
- If you see your child’s eyes are not working together – some or all of the time, wandering up, down in or out – see your doctor promptly. A baby’s eyes should be working together all the time by the age of 4 months… do not wait for it to get better by itself.
When you see your doctor:
- Take any photos with you to explain your concerns.
- Make sure they perform the red-reflex test using an ophthalmoscope.
- If you are still not happy, trust your instinct and see another doctor.
Can You Tell Which two of These four Children Has Eye Cancer?
Strabismus (“squint”, “turned eye”)
Leukocoria (“white pupil”, “white eye glow”, “cat’s eye reflex”)
When “Something” looks like “nothing”…
In each of these two sets, one child has strabismus or leukocoria caused by cancer. The other child has a healthy eye. Can you tell which is which? Find out the answer. If you are concerned about the appearance of your child’s eyes, do not put off asking about it because it seems minor, or wait to see if it will resolve. Please seek medical care early.
A Final Note…
For more than 10 years, with the support of the local community, the ongoing awareness campaigns in Honduras have continued to save more lives, and maybe even eyes and sight. Similarly, awareness campaigns around the world have improved detection, but neither uniformly nor systematically. So there are still many parents who will not be alarmed by seeing a white pupil or a crossed eye in their child. But “if you tell them, they will know”.
About the Author
Sandra Staffieri is the Retinoblastoma Care Co-ordinator at the Royal Children’s Hospital (RCH), Melbourne Australia. Working at the RCH and in private clinics, she has over 35 years’ experience in children’s eye health and disease.
As a Research Fellow and Clinical Orthoptist at the Centre for Eye Research Australia Sandra completed her PhD on delayed diagnosis of retinoblastoma. Her prime focus was to develop and evaluate an information pamphlet for new parents to raise awareness of the important signs of childhood eye disease – particularly strabismus and leukocoria – in the hope this could lead to earlier diagnosis of retinoblastoma.


















My daughter was diagnosed with rb at 18 mths.. in 2009 6 mths chemotherapy didn’t work we were advised to remove her eye but Prof OKeeffe and Prof Galley in Canada recommended laser treatment every 3 wks …the tumour is inactive daughter’s eyesight is perfect she gets a check up every 6 mths.. Éabha is nearly 13 years old now and doing fantastic
The title of this article is what should be enforced, raising awareness about the signs of retinoblastoma as it can save lives, how important it is to attend regular consultations with your optometrist or ophthalmologist of choice, observe children from birth with stop, do not evade any signs, thank you very much for this really important information. https://arisvisionmexico.com/