Visualizing Cancer Treatment
Saturday May 27, 2017 | Abby White, WE C Hope CEO
Have you ever wondered what happens in a child’s eye during retinoblastoma treatment? A range of treatments are used for retinoblastoma. We explore four of the most common eye-saving treatments here. Below each, you will find a link to further information that includes advantages, disadvantages, side effects and questions to ask the doctor.
Laser (photocoagulation)
Several different lasers are used to destroy small tumours in the back of the eye with heat. Tiny tumours may be treated successfully with laser alone. Laser is combined with chemotherapy to treat slightly larger tumours, or those close to the optic nerve or centre of vision.
Chemotherapy flows to cancer cells via the blood. As laser cuts off the tumour’s blood supply, the child receives chemotherapy first. Chemotherapy reduces tumour size so it can be destroyed with laser. This is called consolidation.
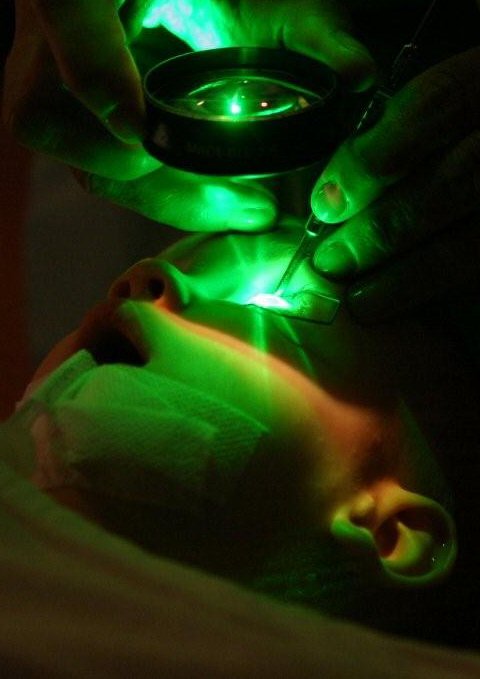
Green laser light flows to the child’s eye.
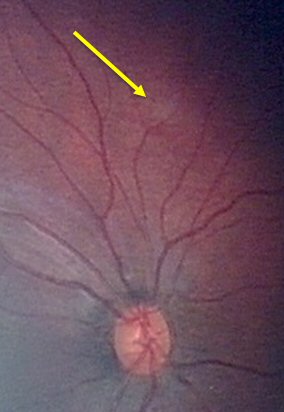
Small tumor before laser (yellow arrow).
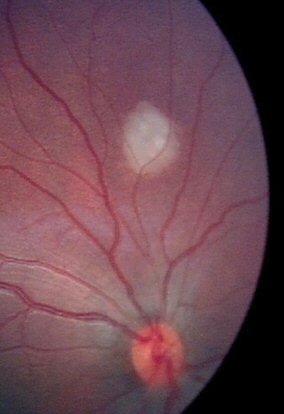
White burns immediately after laser.
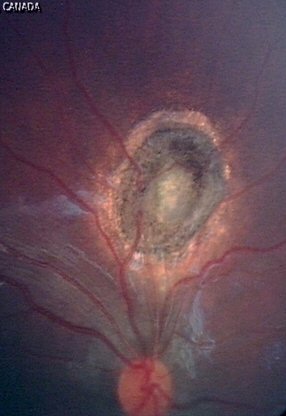
6 months later, flat scar after 4 laser treatments.
Focused beams of light are delivered through an ophthalmoscope. The laser beam is first applied around the tumour’s margin to destroy its blood supply. Subsequent laser burns may be applied directly to the tumour. Repeated treatments are usually necessary to kill the tumours completely
Cryotherapy
Cryotherapy freezes small or relapsed tumours in the periphery of the retina, or when tumours recur after other treatments. Cryotherapy is often used after chemotherapy to reduce tumour size. This is called consolidation.
A single freeze of two spots of cryotherapy to peripheral retina may be given within 48 hours before chemotherapy, to increase penetration of chemotherapy drugs into the vitreous (the fluid core of the eye). This is called prechemotherapy-cryotherapy.
Tumour before freezing.
Ice begins over tumour.
More Ice covering tumour.
Ice covering tumour.
During general anaesthetic, nitrous oxide is applied through a small probe placed against the outside of the child’s eye, opposite the tumour. The tumour is frozen while it is viewed with the indirect ophthalmoscope or retinal camera. As the tumour thaws, ice crystals puncture cell membranes, destroying the cancer cell. At each treatment session, each location is frozen three times, with complete thawing of the tumour in between. This is called triple freeze-thaw cryotherapy. Cryotherapy can be repeated until a flat scar is obtained.
Chemotherapy is the use of anti-cancer drugs. Worldwide, systemic chemotherapy is the most common non-surgical therapy for retinoblastoma. Treatment is directed by a medical or paediatric oncologist (cancer doctor), in collaboration with an ophthalmologist (eye doctor).
A number of drugs are used to treat retinoblastoma. They can be delivered in different ways, and are used either as part of eye salvage therapy or when cancer has spread outside the child’s eye.
Systemic chemotherapy for retinoblastoma is delivered into the bloodstream via an Intravenous (IV) cannula in the arm or hand, or through a central venous catheter.
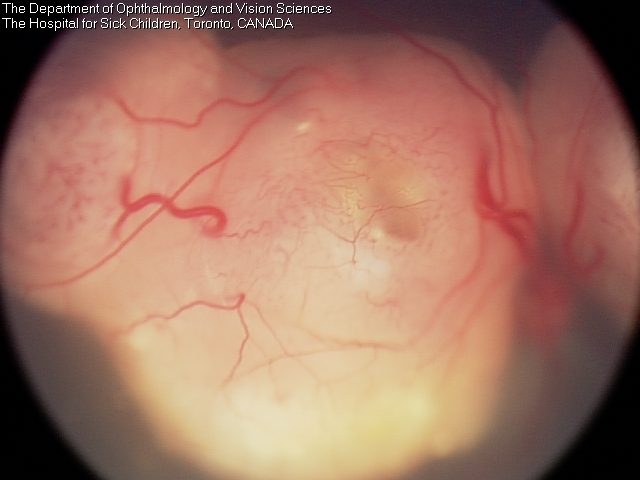
Tumour before systemic chemotherapy.
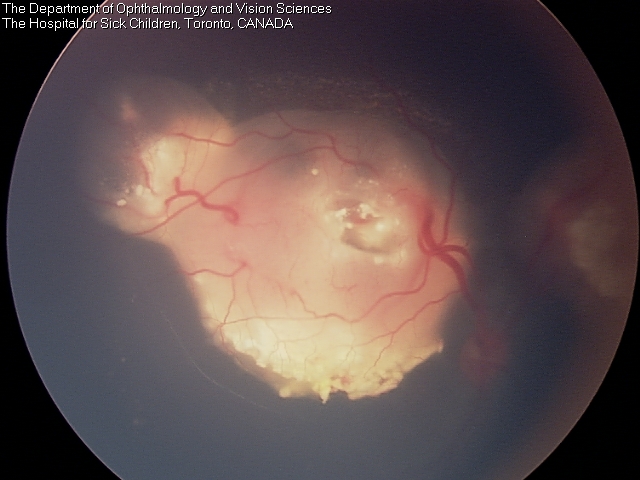
Tumour after a course of systemic chemotherapy.
In eye salvage treatment, chemotherapy shrinks tumours so they can be eradicated with focal therapies. This treatment is usually prescribed when both eyes are affected, there is no risk of cancer escaping the eye and some vision may be saved. Chemotherapy is sometimes used when only one eye is affected and tumours are small, with a good chance of preserving useful vision in the eye. Chemotherapy is vital when cancer has spread outside the eye or has high risk of relapse after enucleation surgery.
A course of intravenous chemotherapy involves a number of cycles. For retinoblastoma, a cycle is usually 2 – 3 days of treatment and a ‘rest’ period of 3 – 4 weeks that allows the body to recover from the effects of the drugs. Most children receive 4-6 cycles. Children with trilateral retinoblastoma or retinoblastoma that has spread to other parts of the body may receive more than a year of chemotherapy.
Intra-Arterial Chemotherapy (IAC)
Intra-arterial chemotherapy is delivered directly into the eye, reached via a catheter inserted into the femoral artery. As a new therapy, IAC should be administered only at a highly experienced retinoblastoma treatment centre that has a clinical research process in place to carefully document the potential benefits and complications.
As primary therapy, IAC can be used to treat medium to large sized intra-ocular retinoblastoma. This treatment must only be used when the optic nerve is clearly seen to be normal, and there is no suggestion of risk that tumour can spread outside the eye.
As salvage therapy, IAC can be effective to control residual, vision-threatening tumour, as long as there is no suggestion of risk that cancer can spread outside the eye.
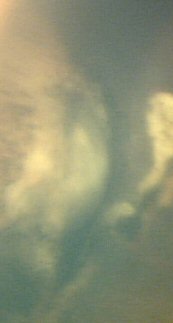
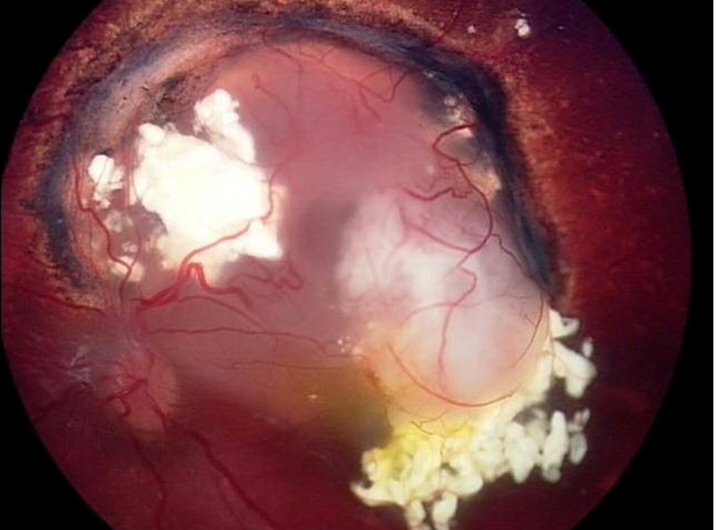
Recurrence after systemic chemotherapy.
The greyish fuzz arising from the white mass to the bottom right of the image is the recurrence.
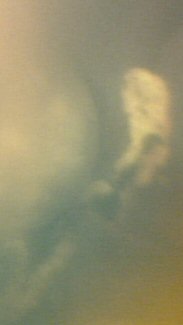
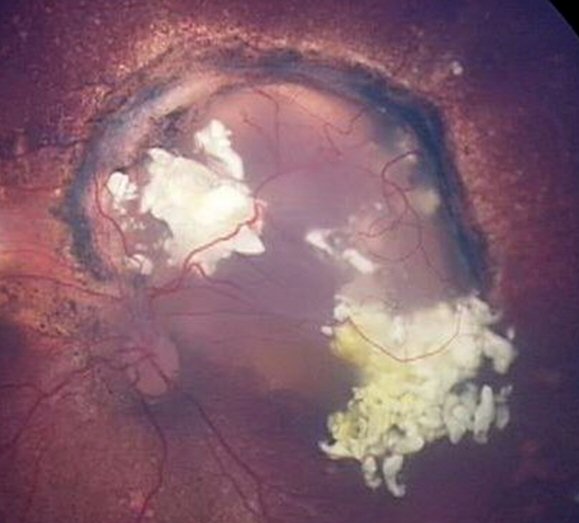
Regression of recurrence after 3 intra-arterial chemotherapy treatments. The tumour is inactive and will be lasered to ensure it is completely dead.
Intra-arterial chemotherapy is administered by an interventional radiologist. Under general anaesthetic, a micro-catheter is threaded through the child’s femoral artery (in the groin) up to the ophthalmic artery carrying blood to the eye to be treated. Fluoroscopy (x-ray imaging) guides the catheter through the body to the ophthalmic artery.
Chemotherapy, either one drug or combinations of melphalan, topotecan, and/or carboplatin, is infused over 30 minutes, after which the catheter is removed. On waking, the child must lay flat for 4-6 hours to prevent bleeding following the catheterization.
Risk of Under Treatment and Relapse Beyond the Eye
When cancer fills the eye, microscopic cancerous cells may invade the optic nerve or the outer layers of the eye, but this will not be seen on eye exam. The only way to know for sure if cancer cells have spread outside the eye is to examine the eye under a microscope after it has been surgically removed. This pathology examination helps doctors know if the child needs systemic chemotherapy to treat cancer outside the eye, to protect their life.
Laser and cryotherapy are used only to treat small, isolated tumours.
Systemic chemotherapy may shrink back tumour that has already spread to key landmarks within the eye (choroid, sclera, optic nerve, anterior chamber). However, without knowing the extent of such spread before treatment, there is a risk of under-treating the cancer. If the eye is later removed, pathological examination of the eye may suggest no further treatment is needed, while tiny cells already floating beyond the eye remain untreated. In this situation, the child would be at high risk of life-threatening relapse months or years later.
Intra-arterial chemotherapy only impacts cancer contained within the eye. It does not treat cancerous cells that may have already spread to the outer layers of the eye or to the optic nerve. A child in this situation may appear to have an excellent response to IAC, while microscopic cancer cells on the eye’s outer layers and beyond continue growing, leading to life-threatening relapse of cancer in the brain or bone marrow some months or year later.
Extraocular retinoblastoma is extremely difficult to treat, even with aggressive chemotherapy and bone marrow transplant. Some children have died following apparently successful IAC treatment that delayed vital life-saving eye removal surgery.
Your Child’s Eyes
Most hospitals that provide sight-saving care now use high definition cameras with which to visualize the child’s eyes. These cameras enable the entire team to view the child’s eye, where previously only the ophthalmologist could see the eye through the ophthalmoscope. Treatments such as laser and cryotherapy can be intricately directed, and viewed during delivery. Photos and video of the eye can be taken during an examination and treatment for later review, reference and comparison.
Ask your child’s doctor to show you images of your child’s tumours at each Exam Under Anaesthetic, and provide you with copies for your records. This additional visual information can be helpful in understanding the cancer, treatment options and results.
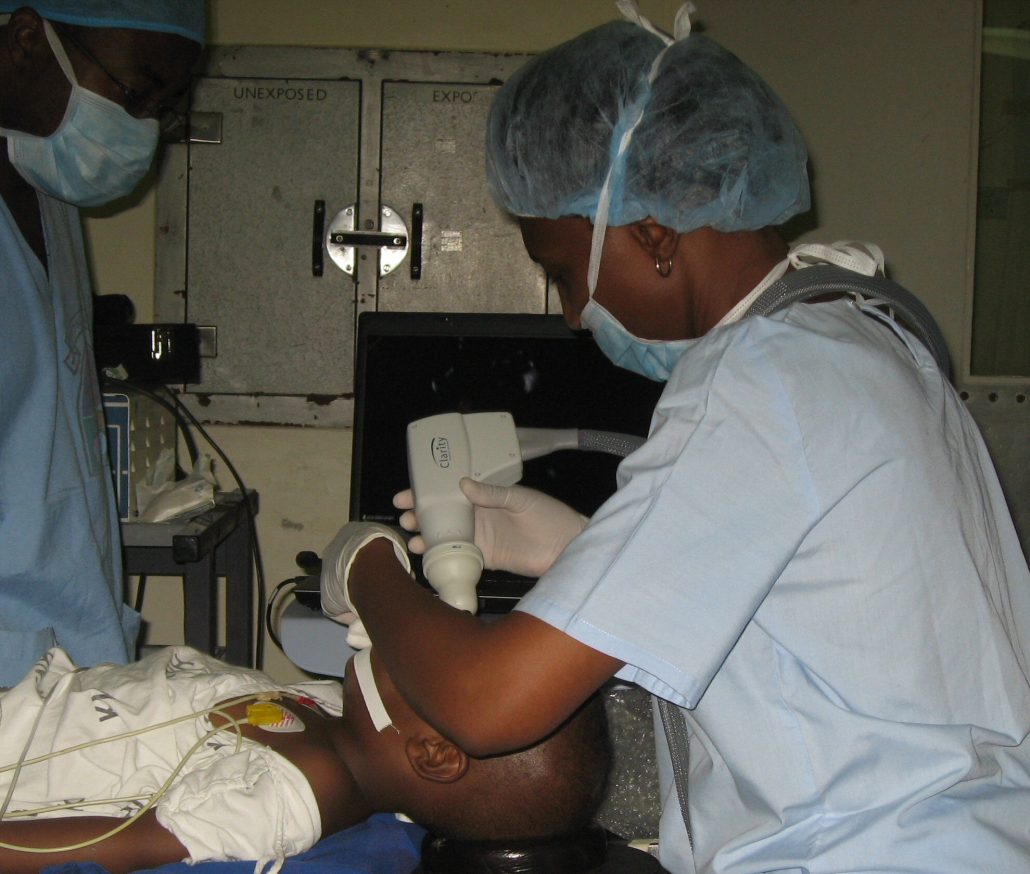
A young boy with retinoblastoma benefits from the RetCam WE C Hope donated to Kenya (the first in Africa).





Leave a Reply
Want to join the discussion?Feel free to contribute!